By Jennifer Richards, LMT 2026
Pregnancy is a time of enormous change for the body. Hormones shift, tissues stretch, and joints become more flexible to prepare for birth. For most people, these changes are temporary and manageable. However, for individuals with Ehlers-Danlos Syndrome (EDS), pregnancy can introduce additional challenges due to the way connective tissue behaves.
EDS is a group of genetic conditions that affect collagen, the protein that helps provide strength and stability to skin, joints, ligaments, and blood vessels. Because collagen is involved in so many structures in the body, pregnancy can affect people with EDS in unique ways.
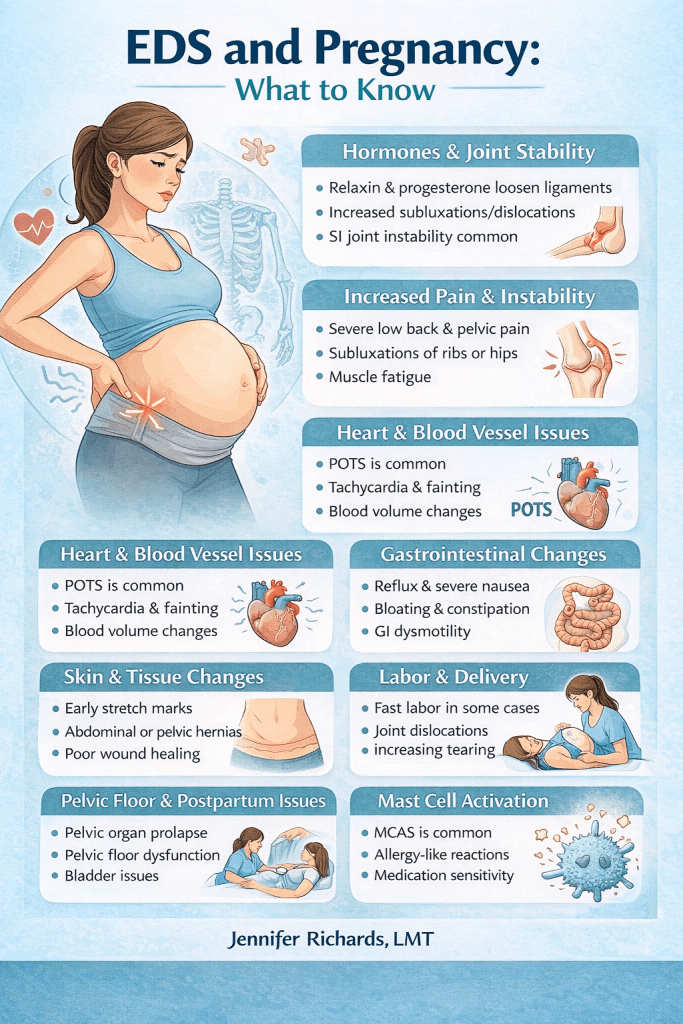
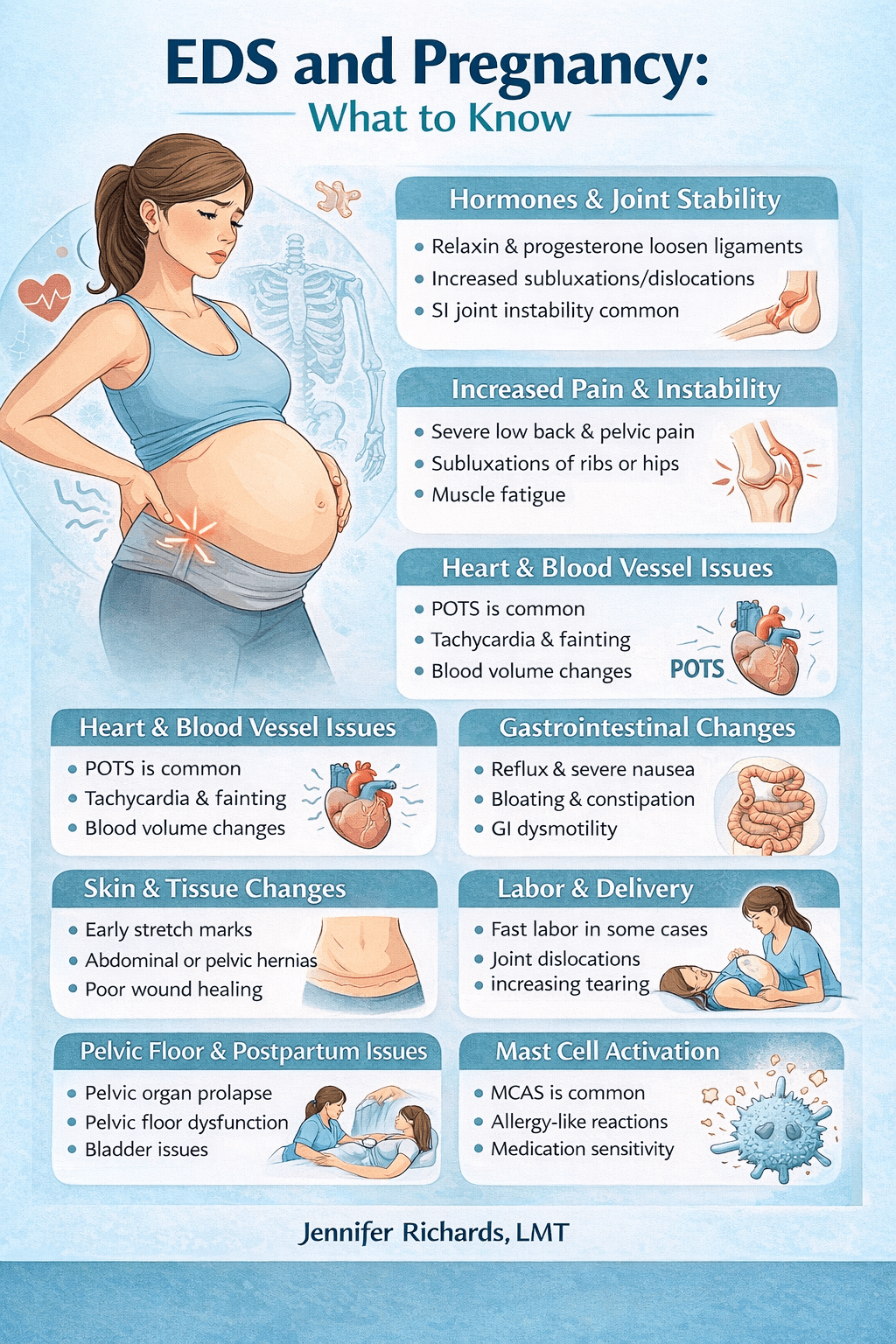
Hormones and Joint Stability
During pregnancy, the body releases hormones such as relaxin and progesterone. These hormones allow ligaments to loosen so the pelvis can expand during childbirth. While this process is completely normal, individuals with EDS already have more flexible connective tissue. The additional hormonal changes can increase joint instability.
Some people notice:
Increased joint looseness
More frequent subluxations or partial dislocations
Sacroiliac (SI) joint instability
Increased muscle fatigue from stabilizing joints
For some hypermobile individuals, joints that were previously manageable may feel significantly less stable during pregnancy.
Increased Pain and Musculoskeletal Stress
As pregnancy progresses, the center of gravity shifts and the growing uterus places additional strain on the spine and pelvis. Because ligaments may not provide adequate stability, muscles often work overtime to support the joints.
Common musculoskeletal symptoms may include:
Low back pain
Pelvic girdle pain
Rib or hip subluxations
Neck and shoulder tension
Increased muscle fatigue
Supportive therapies such as physical therapy, gentle strengthening exercises, massage therapy, and pelvic stabilization can often help manage discomfort.
Cardiovascular and Autonomic Changes
Many individuals with EDS also experience autonomic nervous system conditions such as Postural Orthostatic Tachycardia Syndrome (POTS). Pregnancy naturally increases blood volume and heart rate, which can worsen symptoms in some individuals.
Possible symptoms include:
dizziness when standing
rapid heart rate
fainting episodes
fatigue
Staying well hydrated, using compression garments, and working closely with healthcare providers can help manage these symptoms.
Gastrointestinal Changes
Digestive symptoms are also common in EDS due to connective tissue differences affecting smooth muscle and motility. Pregnancy can intensify these issues.
Some individuals experience:
reflux or heartburn
nausea
bloating
constipation
These symptoms are often manageable with dietary adjustments and medical support.
Skin and Tissue Changes
Because collagen structure is altered in EDS, skin and connective tissues may respond differently during pregnancy. Individuals may notice:
stretch marks appearing earlier or more easily
fragile skin
slower wound healing
increased risk of hernias
These changes vary widely between individuals and between different types of EDS.
Labor and Delivery Considerations
Many people with EDS have safe and healthy deliveries, but there are a few considerations healthcare providers may monitor.
Some individuals report:
faster or precipitous labor
increased tearing
joint instability during certain birthing positions
postpartum bleeding
Because joint stability can vary, it is often helpful for providers to be aware of the condition so labor positioning can be adjusted if needed.
Postpartum Recovery
After delivery, connective tissues are still affected by pregnancy hormones for several months. During this time, people with EDS may be more vulnerable to:
pelvic floor dysfunction
pelvic organ prolapse
joint instability
lingering musculoskeletal pain
Pelvic floor physical therapy can be especially helpful during postpartum recovery.
A Reminder About Individual Experiences
EDS is a spectrum, and pregnancy experiences vary widely from person to person. Some individuals notice increased symptoms, while others find that pregnancy symptoms are manageable with proper support.
The most important factor is having a knowledgeable care team that understands hypermobility and connective tissue disorders.
A Note for Patients Receiving Massage
Massage therapy can be very helpful during pregnancy for people with EDS, but techniques may need to be adapted. Therapists may use lighter pressure, avoid end-range stretching, and provide extra joint support with positioning and bolsters.
If you have EDS and are pregnant, always inform your healthcare providers and bodyworkers so care can be tailored to your needs.
Pregnancy can be a beautiful and empowering experience, even with a connective tissue disorder. With the right support and awareness, many individuals with Ehlers-Danlos Syndrome navigate pregnancy successfully and safely.
Educational Disclaimer
Ehlers-Danlos Syndrome exists on a spectrum, and symptoms vary greatly between individuals. The information presented here is for educational and awareness purposes only. It is not intended to diagnose or treat any medical condition or replace medical care.
Massage therapists do not diagnose medical conditions. Individuals who are pregnant or experiencing symptoms related to hypermobility or connective tissue disorders should consult their healthcare provider for medical guidance.
For more information, go to the Ehlers-Danlos Society