A Gentle Self-Care Guide for Sustainable Practice
Jennifer Richards, LMT
First — You Are Not Broken
If you are hypermobile, you are not fragile.
You are not weak.
And you are certainly not incapable.
But your body does work differently.
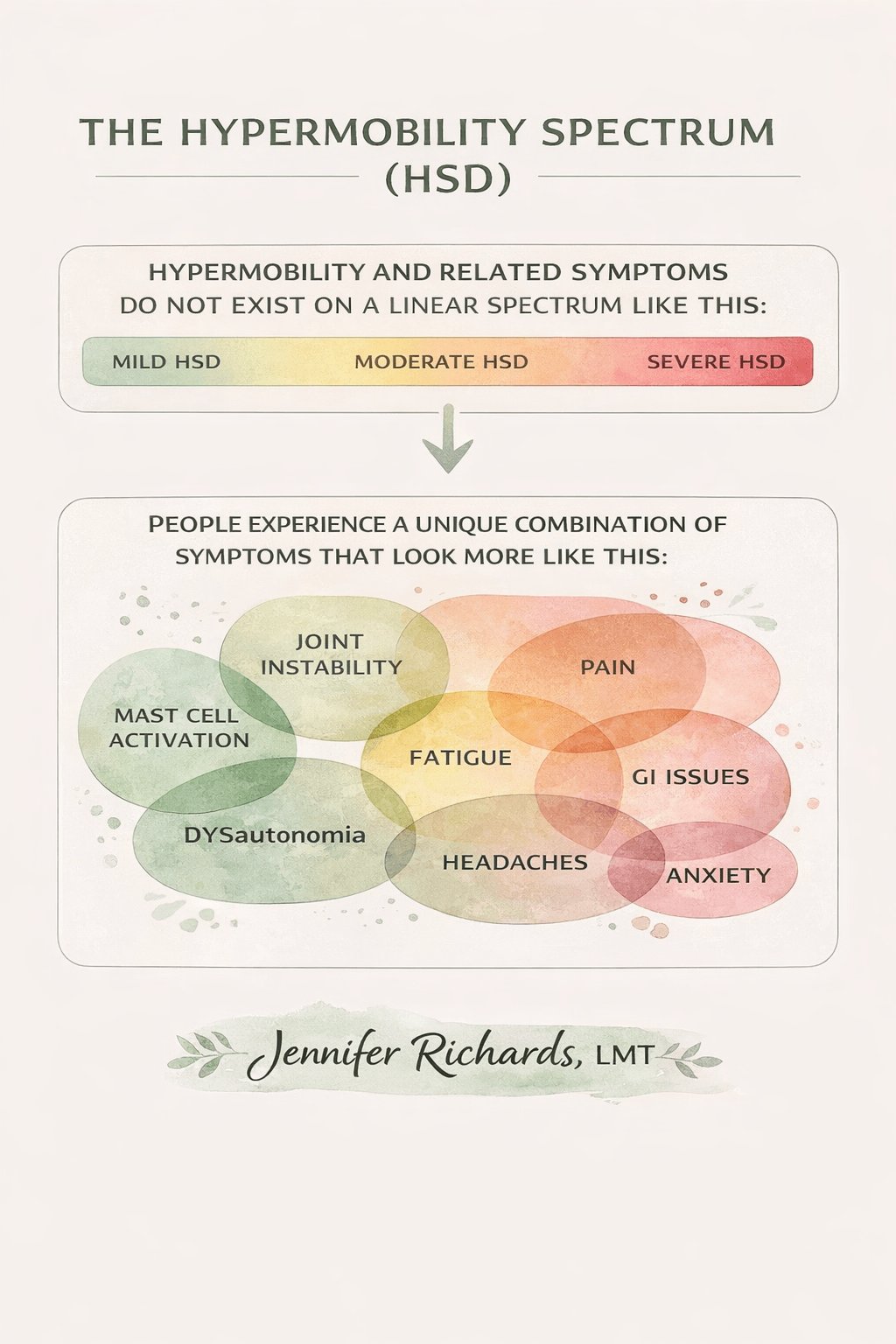
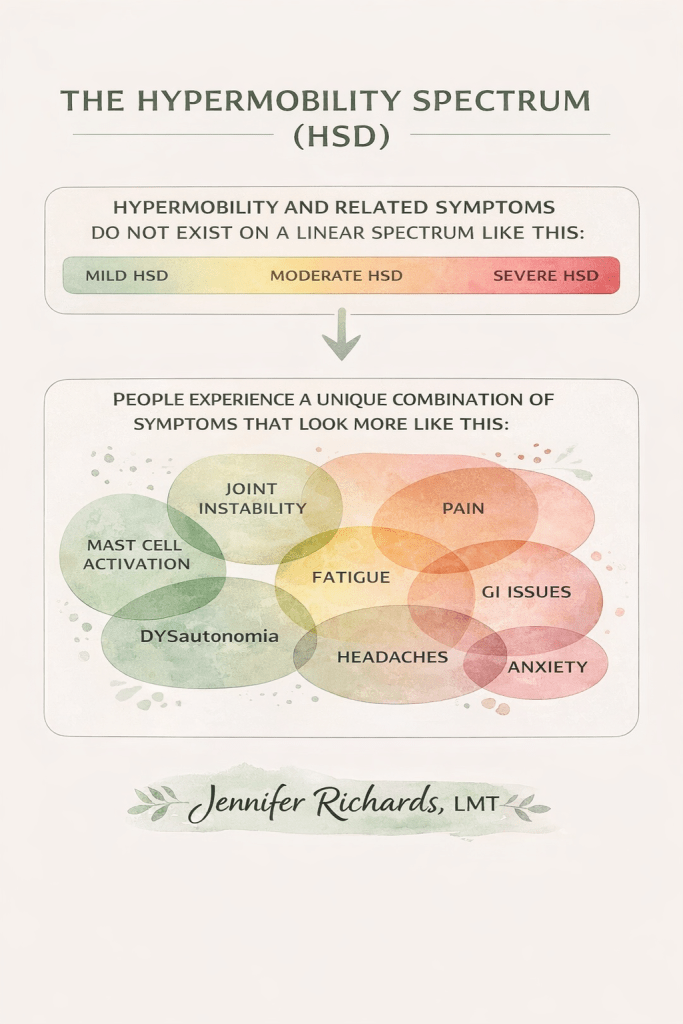
Hypermobility is not just flexibility. It is increased joint range combined with decreased passive stability. Your ligaments are more elastic. Your nervous system works harder to keep you upright. Your muscles often overwork to compensate.
Massage therapy is a physically demanding profession. For hypermobile therapists, sustainability requires intention.
This guide is about protecting your longevity — not limiting your potential.
🥄 Energy Is Real: The Spoon Theory
The Spoon Theory, described by Christine Miserandino, explains energy as a limited resource.
Some days you wake up with:
20 spoons Other days: 7
Massage uses:
Postural endurance
Grip strength
Micro-stabilization
Emotional presence
Nervous system regulation
You cannot out-discipline a connective tissue disorder.
Consider:
Fewer back-to-back deep sessions Alternating lighter sessions between heavier ones Built-in recovery days Honest scheduling
Energy management is not laziness. It is strategy.
😴 Sleep Is Non-Negotiable
Hypermobile bodies:
Repair tissue more slowly
Experience higher sympathetic tone
Often have dysautonomia
Fatigue more quickly
Sleep is when:
Collagen turnover occurs
Muscles recover
The nervous system recalibrates
Helpful supports:
Consistent sleep and wake times
Cervical pillow that maintains neutral alignment
Body pillow for joint support
Magnesium glycinate (if tolerated and provider-approved)
Cooling sheets or breathable fabrics if temperature regulation is difficult
You cannot “push through” chronic sleep deprivation. It will always collect interest.
🥗 Nutrition for Stability
We are not trying to shrink your body.
We are trying to support your tissues.
Focus on:
Adequate protein (for muscle and collagen support)
Vitamin C (collagen synthesis)
Omega-3 fatty acids Electrolytes (especially with dysautonomia)
Whole, minimally processed foods
Limit:
Ultra-processed foods
High sugar intake
Excess alcohol
Excess caffeine (particularly if you experience tachycardia or POTS-like symptoms)
Possible supplements (discuss with a healthcare provider):
Magnesium
Vitamin C
Electrolytes
Collagen peptides (evidence is mixed, but may support some individuals)
Food is not punishment or control. It is structural support.
🏋️ Exercise: Stability Over Stretching
You do not need more stretching.
Hypermobility requires:
Proprioception
Controlled strengthening
Stability at mid-range
Slow tempo movements
Educator Jeannie Di Bon emphasizes safe strengthening for hypermobile bodies — focusing on control rather than end-range flexibility.
Helpful strategies:
Closed-chain exercises
Isometric holds
Deep neck flexor work
Glute medius strengthening
Scapular stabilization
Core control
Avoid:
Repeated end-range loading Locking knees or elbows Aggressive yoga “No pain, no gain” approaches
Strength protects you. Stretching without control destabilizes you.
🖐️ Support Tools That Make a Difference
Ring splints: Prevent finger hyperextension. Reduce joint fatigue during sessions.
Compression garments: Helpful for POTS/dysautonomia
Cooling scarves or neck wraps: Helpful for mast cell flares or temperature dysregulation
Proper footwear: Firm arch support. Replace shoes regularly Avoid overly flexible or worn footwear.
Anti-fatigue mats: Reduce ankle and knee strain Protect your lower back
Table height: Slightly higher than standard recommendation Prevents elbow locking and shoulder strain.
Small environmental changes create long-term protection.
💆 Work Smarter, Not Harder
Your hands are not your only tools.
Consider:
Forearm techniques
Assisted tools when appropriate
Micro-breaks between clients
Gentle wrist CARs between sessions
Hydration between clients
Rotating modalities
You are allowed to design your schedule around sustainability.
🫀 Nervous System Regulation
Many hypermobile individuals live in a heightened sympathetic state.
Add:
Slow diaphragmatic breathing
Gentle vagal toning practices
Time outdoors
Real rest (not scrolling)
HRV tracking if helpful
If you experience:
Lightheadedness
Tachycardia
Temperature instability
Brain fog
These may reflect autonomic dysfunction, not anxiety or weakness.
🛏️ Joint Protection at Home
Recovery continues after work.
Helpful supports:
Body pillow for hip and shoulder alignment
Cervical support pillow
Avoid prolonged end-range positions
Avoid sleeping with arms overhead
You heal while you rest.
🚫 What to Avoid
Pushing through pain
Competitive comparison culture
Locking joints during treatment
Excessive caffeine to compensate for fatigue
Living in chronic sleep debt
Ignoring autonomic symptoms
Sustainability is the goal. Not martyrdom.
🌿 You Are Not Weak
Many hypermobile therapists:
Overperform Overdeliver Overcompensate Crash privately
Pacing is not giving up.
It is professional maturity.
Longevity is the real measure of success in this profession.
When to Seek Support
Consider evaluation if you experience:
Recurrent joint instability
Frequent subluxations
Persistent tachycardia
Severe fatigue
Repeated injury
Appropriate referrals may include:
Physical therapy familiar with hypermobility
Cardiology (if dysautonomia suspected)
Rheumatology
Genetics Pelvic floor PT
Early support prevents burnout and injury.
Final Thoughts
You deserve to practice in a way that protects your future.
Hypermobility does not disqualify you from massage therapy.
But it does require wisdom.
Your body is not an obstacle.
It is information.
Listen to it.
Disclaimer
This guide is for educational purposes only and does not replace individualized medical advice. Hypermobility and connective tissue disorders exist on a spectrum. Consult a qualified healthcare provider before making changes to exercise, supplementation, bracing, or dietary practices. What is appropriate for one person may not be appropriate for another.